
100 Years of Insulin
World Diabetes Day 2021 coincided with the centenary anniversary of the ground-breaking discovery of insulin. We take a closer look at the research breakthrough that has improved, and in many cases saved, the lives of people living with diabetes ever since.
2021 marked the 100th year anniversary of the discovery of insulin – a landmark moment for people living with diabetes worldwide.
The discovery is still considered to be one of the most significant medical developments in history, which transformed diabetes from a fatal disease to a manageable condition and prolonged life for decades.
The first successful test of insulin was conducted at the University of Toronto by a small team of researchers led by Sir Frederick Banting. The result marked the beginning of a wave of successful trials on people living with diabetes.
Within months, mass-production of the life-saving drug began across North America and was soon shipped to the rest of the world.
A century later, insulin remains the only available treatment for type 1 diabetes.

Picture: Charles Best (left) and Sir Frederick Banting (right) at the University of Toronto in 1925. (Thomas Fisher Rare Book Library, University of Toronto).
The pre-insulin era
Prior to the discovery of insulin, life was incredibly difficult for people living with diabetes.
The condition was first recorded as far back as 1550BC in ancient Egypt, when physicians identified the symptoms of an unknown illness that caused thirst, excessive urination and eventually death.
As thousands of years passed, medical science failed to develop any effective treatment for the condition. During this time, a diagnosis of diabetes was fatal.
Patients were expected to live only one or two years before entering diabetic ketoacidosis (DKA) and eventually succumbing to the condition.
Only in the nineteenth century did physicians begin to develop a better understanding of diabetes and how to control its effects.
The discovery that carbohydrate and sugar intake was connected to diabetes caused physicians to focus on diet to control diabetes.
The approaches physicians took varied significantly. Apollinaire Bouchardat, a French pharmacist and diabetologist, introduced a popular sugar-free diet, which often resulted in his patients reducing the amount of sugar discovered in their urine.
However, his fellow countryman and renowned physician Pierre Adolphe Piorry, believed the opposite. He encouraged people with diabetes to increase their calorific consumption to negate the loss of calories from diabetes.
Both of these diets were commonly experimented with, most of which resulted in the rapid decay of their patient’s health.
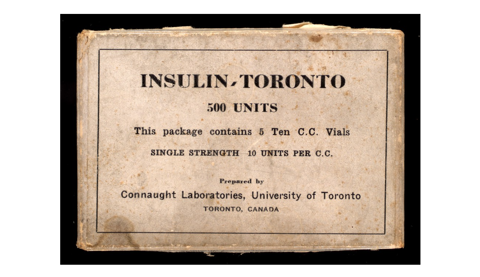

Picture: Some of the earliest produced insulin available for public use. (Thomas Fisher Rare Book Library, University of Toronto).
In the early years of the twentieth century, scientists continued to focus treating diabetes with diets.
Two of the most prominent diabetes specialists in America, Frederick M. Allen and Elliott P. Joslin, introduced a severe restricted diet to prolong the life of those living with diabetes.
Commonly referred to as “starvation diets,” Allen and Joslin prescribed a daily calorific intake of just 500 calories, along with periods of intense fasting.
The discovery closes in
Just a few decades before insulin was discovered, a loose scientific understanding of diabetes began to emerge.
German scientist Paul Langerhans correctly identified that the pancreas served two primary functions. He noted that the organ secretes some sort of hormone.
Langerhans study of the pancreas led to the discovery of the islets of Langerhans, a group of insulin-producing cells in the pancreas, also known as islet cells.
In 1889, two German scientists correctly identified a link between the pancreas and diabetes.
The discovery of insulin was now on the horizon, and these studies would prove crucial in the breakthrough at the University of Toronto.

Picture: Charles Best (left) and Sir Frederick Banting (right) at the University of Toronto in August 1921. (Thomas Fisher Rare Book Library, University of Toronto).
Discovery
In November 1920, Canadian surgeon Frederick Banting began exploring how insulin could be extracted from islet cells in the pancreas.
He started working at the University of Toronto, with support from Professor J. J. R. Macleod, a physiology professor and global expert in diabetes.
Macleod provided Banting with a laboratory and assigned Charles Best, a promising research student, to assist Banting with his experiments.
In May 1921, Banting and Best began removing the pancreas from research dogs and performed pancreatic duct ligation to separate insulin-producing cells from the rest of the pancreas.
By November, they successfully extracted insulin from the pancreas and successfully treated a dog with diabetes for 70 days.
The promising results allowed for human trials to be considered for the first time. Biochemistry professor James Collip was introduced to purify the insulin, allowing it to be safely administered to people living with diabetes.
First person to be treated with insulin
On 11 January 1922, Leonard Thompson became the first person to be treated with insulin.
Leonard was 14 and had been living with diabetes for two and half years before being admitted to Toronto General Hospital. Like many diabetes patients, he was severely ill and weighted just 65 pounds.
Leonard had been placed on a “starvation diet” by his doctors, which restricted him to just 450 calories a day.
The first dose of insulin administered to Leonard lowered his blood glucose levels by around a quarter and reduced the level of glucose in his urine.
However, due to impurities in the insulin, an abscess developed around the injection site and Leonard’s ketone levels remained dangerously high.
Collip continued to purify the insulin and achieved success within weeks.
On 23rd January, Leonard received his second dose of insulin.
Within 24 hours, his blood glucose levels dropped by around 77% and his physical appearance improved remarkedly.
Just three months later, he “looked better” and “felt stronger” and was discharged from hospital.
Picture: Leonard Thompson a few years after he became the first person to receive insulin. He lived for 13 years on insulin and died April 20, 1935 at the age of 27. His death was due to broncho-pneumonia and complications from diabetes. (Thomas Fisher Rare Book Library, University of Toronto).



Pictures: James Collip (left) as a graduate student in 1914 and Teddy Ryder (right) sometime after he received insulin. (Thomas Fisher Rare Book Library, University of Toronto).
Leonard was not the only success story. Five-year-old Teddy Ryder was among the first group of patients treated by Banting and Best’s insulin at Toronto General Hospital in 1922.
One of the youngest patients to be treated with insulin, Teddy weighed only 26 pounds and could hardly move before the breakthrough in Toronto.
With access to insulin, Teddy made a remarkable recovery, and lived for a further 77 years.
Worldwide impact
The remarkable success of the first human trials led to rapid clinical deployment of insulin therapy across the globe.
In 1923, the American pharmaceutical company Lilly began to ship the first commercial stock of insulin across North America.
Just one month later, Nordisk Insulin Laboratory started producing insulin in Denmark and began shipping vials globally.
The incredible work of Banting, Best, Macleod and Collip marked the end of diabetes as a fatal condition. In recognition of their achievement, Banting and Macleod were awarded the Nobel Prize in Physiology or Medicine.
They divided their prize money equally with Best and Collip, who had both been overlooked despite their significant contributions.
Finally, people with diabetes had access to a treatment which could improve the quality and prolong the duration of their life by decades.
The development of insulin had only just begun. Over the next few decades, the quality of insulin and how it was administered improved significantly.
The introduction of synthetic human insulin in 1982 was a significant milestone in the treatment of diabetes. It allowed for insulin to be genetically engineered in laboratories, ending the practice of extracting insulin from cattle and pigs.

Picture: Sir Frederick Banting at this desk in 1926 (Thomas Fisher Rare Book Library, University of Toronto).
Present/future
The discovery remains one of the most important medical breakthroughs in history. To the present day, millions of people still rely on insulin. It ignited a century of development in diabetes care and has undoubtedly saved millions of lives.
At DRWF, we think it is time for the next big breakthrough; our ultimate goal is to find a cure for diabetes. In pursuit of this, we fund some of the best and brightest diabetes researchers, whose work improves our understanding of diabetes. Our funded research explores new treatments; develops self-management strategies; and seeks out potential cure pathways.
The dedication and commitment of our diabetes research community is second to none.
Through our awareness and educational support programmes, we enable people to learn more about diabetes, providing the tools to motivate, empower and engage in a pro-active approach to good self-care.
Every day, we do our utmost to ensure that people living with diabetes are ‘staying well until a cure is found…’
Read more about type 1 diabetes
Support DRWF by making a donation here
Find out more about DRWF-funded research here
Find out more about DRWF fundraising here
For latest update follow DRWF on Facebook, Instagram and Twitter
To receive the charity’s latest bulletins as they become available, please sign up here
Read DRWF diabetes information leaflets here
Join the Diabetes Wellness Network here
I would like to make a regular donation of
There are lots of ways to raise money to support
people living with all forms of diabetes.
Bake, Swim, Cycle, Fly ... Do It For DRWF!
Fundraise with us
Recent News


