
The psychological impact of diabetes
Understanding the symptoms of depression and how to maintain good self-management of diabetes.
Having diabetes can take its toll, with the different aspects of self-management often feeling overwhelming. The responsibility for managing diabetes lies almost entirely in the hands of the person with this life-long condition.
People with different types of diabetes often have distinctive psychosocial needs. This article focusses on type 2 diabetes which is the most common form of the condition.
Impact on quality of life
The personal costs for those with type 2 diabetes are many. It can impact on relationships, on working and social life, and on psychological well-being, with a consequent effect on overall quality of life.
Constant monitoring, following a healthy diet and finding time for exercise can all lead to improved mental and emotional health.
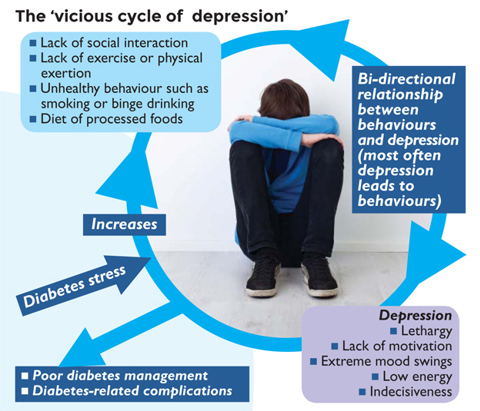
The opposite may also be true; feeling depressed or anxious can lead to poor control of diabetes. This has been demonstrated in many studies and reviewed by Frank Snoek and his colleagues for The Lancet. The cyclical relationship between mental health and diabetes is illustrated in Figure 1 (page 6).
Depression
People with diabetes are up to three times more likely to report symptoms of depression and these can be debilitating. For type 2 diabetes, £1.8 billion of additional costs to the NHS can be attributed to poor mental health. However, less than 15% of people with diabetes have access to psychological support, in spite of the fact that psychological support improves health and cuts costs by 25%.
Poor mental and emotional well-being can lead to feeling less inclined to monitor blood glucose levels which then impact on self-management and diabetes control. People who feel depressed often feel lethargic and so are less likely to exercise. Diet is also very often affected with less healthy foods and more alcohol consumed. In addition, sleep is often affected (problems sleeping are one of the symptoms of depression), which can have a serious impact on overall quality of life.
Figure 1: The cyclical nature of the relationship between depression and diabetes (adapted from Diabetes UK)
Symptoms of depression include:
- Feeling sad/depressed mood
- Lack of interest/enjoyment in daily activities
- Inability to sleep
- Early waking
- Tiredness/lack of energy
- Loss of appetite
- Feelings of guilt/worthlessness
- Recurrent thoughts about death/suicide
Emotional distress
People with diabetes may also experience diabetes-related emotional distress and although there is a strong association between distress and depression, many people only report one or the other.
Symptoms of diabetes-related distress include constantly worrying about blood glucose levels or the risk of getting diabetes complications, feeling angry about living with diabetes, and feeling guilty when going off track with managing diabetes self-care.
Distinguishing between symptoms of depression or diabetes-related distress through discussion with the diabetes nurse or GP, can help to decide what the most appropriate follow-up care should be offered.
For example a referral for counselling or other ‘talking therapies’, or diabetes education. The ‘vicious cycle’ (as described in figure 1) can be broken if appropriate support is given.
Importance of well-being
The importance of psychological and emotional well-being has now been recognised by not only Diabetes UK, but the National Institute for Health and Care Excellence (NICE) and there are guidelines for the management of diabetes and depression when they occur together.

NHS England has also recognised the importance of good mental health, advocating a holistic approach to care for people with diabetes which includes consideration of mental and emotional well-being as well as physical health (NHS England 2018). Diabetes UK has recommended that ever person with diabetes should be in receipt of 15 healthcare essentials - including getting psychological and emotional support, and that receiving more integrated care would improve outcomes and quality of life. This, they say, would also subsequently reduce healthcare costs.
A ‘stepped care’ approach to treating depression has been recommended by NICE which organises provision according to what is seen as the patient’s specific needs.
Identifying the symptoms
When someone goes to their GP to discuss feeling depressed or anxious, identification of symptoms starts with two questions:
1. During the last month, have you often been bothered by feeling down, depressed or hopeless?
2. During the last month, have you often been bothered by having little interest or pleasure in doing things?
If the answer is ‘yes’ to either of these questions, then further questions are asked in order to decide on the next step, and this is usually based on the severity of symptoms.
What support is available?
A service available to all those identified as having depressive symptoms is the Improving Access to Psychological Therapies (IAPT) service. GPs usually make the referral, however self-referral is also an option. The IAPT service consists of talking therapies such as cognitive behavioural therapy.
NICE guidelines, based on existing evidence, also recommend the use of physical activity groups, motivational interviewing, and group or family therapy.
Some people prefer group rather than individual support as it can promote a sense of belonging, sharing stories and feeling less isolated.
A recent systematic review of studies investigating the impact of different treatments in people with diabetes found that both psychological and pharmacological interventions had a moderate effect on depressive symptoms, but had no impact on quality of life. NICE are currently updating their guidance and evaluating the evidence which can inform their recommendations.
Specific guidelines for supporting people with long-term conditions (including diabetes) have only very recently (April 2018) been developed and are yet to be widely available. At the same time, direct access to psychological support in primary or secondary diabetes clinics remains scarce.
There is often a lack of confidence in talking about depression or other psychological and emotional problems, on the part of both the GP and the person with diabetes.
The treatment of diabetes and its physiological consequences is often seen as the main priority of care, with psychological well-being further down the list, and worries about the most appropriate service to offer or receive are common.

Don’t be afraid to ask for help
Asking for help with psychological problems can be difficult. Mental health problems still carry a stigma which can influence whether or not symptoms are expressed.
The language used within clinical settings can also influence the discussions. Using words such as ‘adherence’ or ‘compliance’ with treatment can have serious negative effects. Conversely, using non-discriminatory words can open up conversations and help identify the particular needs of the person with diabetes.
More support is needed
In summary, diabetes can have a serious psychological and emotional impact, and can affect self-management as well as the individual’s quality of life. A range of psychological problems can occur including depression, anxiety and diabetes-related distress.
Diabetes care service providers have acknowledged the extent of this problem and advocate a holistic approach to care which includes consideration of both physical and mental health.
It is recommended that psychological well-being is addressed in clinical consultations so that the most appropriate and person-centred care is provided, however there remains a shortage of specialist support.
More information
The above is a sample article from a recent Diabetes Wellness News – it was originally published in the March 2019 issue of Diabetes Wellness News (reviewed within 18 months from publication date). Source references are available on request.
For more information about subscribing to Diabetes Wellness News please visit here
Support DRWF by making a donation here
Find out more about DRWF-funded research here
Find out more about DRWF fundraising here
For latest update follow DRWF on Facebook, Instagram and Twitter
To receive the charity’s latest bulletins as they become available, please sign up here
Read DRWF diabetes information leaflets here
Join the Diabetes Wellness Network here
I would like to make a regular donation of
There are lots of ways to raise money to support
people living with all forms of diabetes.
Bake, Swim, Cycle, Fly ... Do It For DRWF!
Fundraise with us
Recent News


